Denial Prevention TESTING
Faster claim management. Financial success. Less stress.


We’re Here to Advocate for You
What is Denial Prevention?
Denied claims create costly delays and administrative burden – but with TMC, you’re not facing them alone. Our Denial Prevention & Management services are built into every therapy partnership, helping you avoid issues before they start and resolve them efficiently when they do.
From navigating audits and responding to ADRs to managing appeals and tracking trends, our team works side by side with your billing and therapy departments to protect earned revenue and reduce disruption. We stay ahead of CMS and payer requirements so your staff can stay focused on care, and not paperwork.
EXPANDED SUPPORT FOR PT, OT & ST CLAIM DENIAL PREVENTION
Therapy claim denials don’t just impact revenue, they disrupt care delivery. TMC provides proactive denial prevention strategies across physical therapy (PT), occupational therapy (OT), and speech-language pathology (ST), helping facilities identify issues before claims are submitted.
From documentation gaps to authorization errors, our team addresses the root causes of denials to support stronger compliance, improved clean claim rates, and more predictable reimbursement.
What We Help You Prevent
- Incomplete or non-compliant therapy documentation
- Medical necessity denials across PT, OT, and ST services
- Authorization and timing issues that delay reimbursement
- Increased risk of ADRs and payer audits
Proactive Insight, Powered By Technology
By combining data-driven insights with clinical expertise, we help your team stay ahead of CMS updates and evolving payer requirements, reducing preventable denials before they occur.
Tailored Support For Every Care Setting
Our team integrates directly with your staff to strengthen documentation practices, streamline appeals, and support therapy-specific compliance across PT, OT, and ST service lines.
Built On Compliance And Clinical Oversight
Every claim is supported by clear clinical evidence, helping minimize denials, avoid ADRs, and protect long-term revenue integrity.
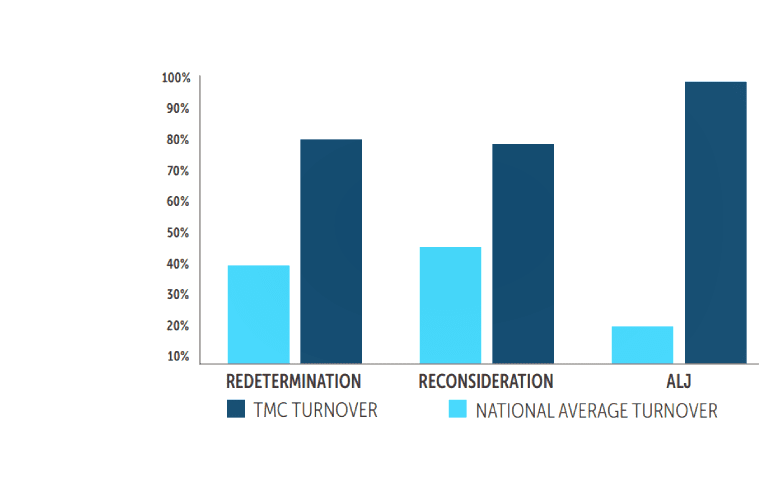
Prevention & Resolution
When denials happen, TMC takes the lead. Our team manages the entire appeals process - from gathering documentation and preparing responses to submitting directly to payers. We act quickly, communicate clearly, and handle the follow-through, so your billing and clinical teams don’t have to. It’s hands-on support that removes the hassle, protects your reimbursement, and gives you peace of mind.
Frequently Asked Questions
Do you support all therapy disciplines?
Yes. TMC provides denial prevention and appeals support for physical therapy (PT), occupational therapy (OT), and speech-language pathology (ST) across all care settings, including skilled nursing, outpatient, and hospital environments.
How does TMC assist with therapy claim denial prevention?
TMC employs a multi-faceted approach that includes comprehensive documentation audits, real- time clinical oversight, and the use of proprietary software to identify potential red flags before claims are submitted. Our nearly 30 years of experience allow us to anticipate payer shifts and ensure your facility remains compliant while protecting its bottom line.
What sets your denial prevention services apart from other providers?
Our services are rooted in a partnership-focused model that emphasizes integrity and service
excellence. Unlike standard billing services, TMC provides clinical education and flexible support tailored to the specific needs of skilled nursing facilities and outpatient clinics, ensuring that therapy claim denial prevention is integrated into the daily workflow.
Can TMC help manage appeals for claims that have already been denied?
Yes, our team of experts provides robust support for managing appeals and navigating the
complexities of ADRs. By analyzing the reasons behind existing denials, we not only work to
recover earned revenue but also implement long-term strategies to prevent similar issues from
occurring in the future.
What role does technology play in your denial prevention strategy?
We utilize advanced proprietary software designed to track denial trends and monitor compliance metrics in real-time. This technological edge provides our partners with data-driven insights, allowing for proactive adjustments to documentation and billing practices that significantly reduce the risk of claim rejections.




